How Peripheral Artery Disease Affects Foot and Ankle Skin
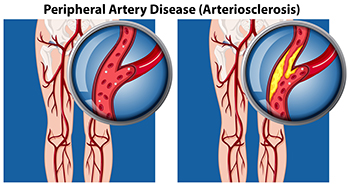
Peripheral artery disease, or PAD, reduces blood flow to the lower limbs, limiting the oxygen and nutrients needed to keep skin healthy. In the feet and ankles, this often leads to dryness, thinning, and increased sensitivity. Skin may appear shiny, pale, or cool to the touch, and hair growth can diminish. Even minor cuts or pressure areas may heal slowly because circulation is impaired. Over time, poor blood supply increases the risk of skin breakdown, ulcers, and infection, especially when combined with reduced sensation. Color changes, cracking, or persistent redness should not be ignored, as they may signal worsening circulation. Wearing proper footwear, daily skin checks, and prompt care of small injuries are essential for protection. If changes in foot or ankle skin are noticed, it is suggested that you see a podiatrist for a proper diagnosis and appropriate treatment.
Peripheral artery disease can pose a serious risk to your health. It can increase the risk of stroke and heart attack. If you have symptoms of peripheral artery disease, consult with Ambrose Su, DPM from Cascade Foot Clinic. Our doctor will assess your condition and provide you with quality foot and ankle treatment.
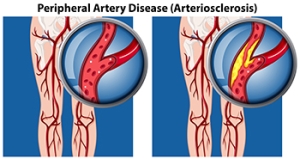
Peripheral artery disease (PAD) is when arteries are constricted due to plaque (fatty deposits) build-up. This results in less blood flow to the legs and other extremities. The main cause of PAD is atherosclerosis, in which plaque builds up in the arteries.
Symptoms
Symptoms of PAD include:
- Claudication (leg pain from walking)
- Numbness in legs
- Decrease in growth of leg hair and toenails
- Paleness of the skin
- Erectile dysfunction
- Sores and wounds on legs and feet that won’t heal
- Coldness in one leg
It is important to note that a majority of individuals never show any symptoms of PAD.
Diagnosis
While PAD occurs in the legs and arteries, Podiatrists can diagnose PAD. Podiatrists utilize a test called an ankle-brachial index (ABI). An ABI test compares blood pressure in your arm to you ankle to see if any abnormality occurs. Ultrasound and imaging devices may also be used.
Treatment
Fortunately, lifestyle changes such as maintaining a healthy diet, exercising, managing cholesterol and blood sugar levels, and quitting smoking, can all treat PAD. Medications that prevent clots from occurring can be prescribed. Finally, in some cases, surgery may be recommended.
If you have any questions, please feel free to contact our office located in Bend, OR . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Peripheral Artery Disease
Peripheral artery disease (PAD), or peripheral arterial disease, is a circulatory problem in which there is a reduction of blood flow to the limbs due to narrowed arteries. When peripheral artery disease develops, the extremities do not receive enough blood flow; this may cause symptoms to develop such as claudication, or leg pain when walking. The legs are the most common site of peripheral artery disease.
Claudication, or leg pain when walking, is one of several symptoms that can develop due to peripheral artery disease. Other symptoms caused by the disease include painful cramping in the hips, thighs, or calves after certain activities; leg numbness or weakness; coldness in the lower leg or foot; sores on the lower extremities that do not heal; hair loss on the lower extremities; and a missing or weak pulse in the lower extremities. In more severe cases, pain may even occur when the body is at rest or when lying down.
Peripheral artery disease is typically caused by atherosclerosis, a condition in which fatty deposits build up in the arterial walls and reduce blood flow. Smoking, diabetes, obesity, high blood pressure, and high cholesterol are some of the risk factors for peripheral artery disease.
If you are experiencing pain, numbness, or other symptoms in the lower extremities, see your healthcare professional immediately. Diagnosed peripheral artery disease can be treated with various medications, angioplasty and surgery, exercise programs, or alternative medicine. It is important to consult a healthcare professional to determine the best treatment for you.
Types of Fungal Toenail Infections
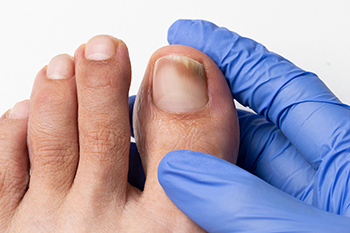
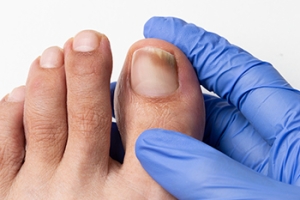
Fungal toenail infections develop when microscopic fungi enter small cracks in the nail or surrounding skin and slowly multiply in the warm, moist environment inside shoes. Several distinct types affect toenails. A distal subungual infection is the most common. It begins at the tip or sides, causing yellow or white streaks and thickening beneath the nail. White superficial infection involves the surface layers, producing chalky patches that make the nail rough and crumbly. Proximal subungual infection starts near the cuticle and spreads outward. It is sometimes linked with weakened immunity or prior injury. Yeast-related infections may inflame the surrounding tissue and loosen the nail from its bed. A podiatrist confirms the diagnosis using nail samples and determines the specific organism before prescribing medical antifungal therapy, nail procedures, or advanced management for damaged nails. If you have a fungal toenail infection, it is suggested that you make an appointment with a podiatrist for an exam, diagnosis, and treatment.
For more information about treatment, contact Ambrose Su, DPM of Cascade Foot Clinic. Our doctor can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please contact our office located in Bend, OR . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
How to Treat Your Toenail Fungus
While not a serious issue, toenail fungus, or onychomycosis, can be an embarrassing and uncomfortable condition to experience. Toenail fungus is often caused from public areas that harbor fungi and improper cleaning/drying of the foot. Once infected, the fungus grows deeper into the nail and can be very hard to get rid of.
There are different types of fungus that cause toenail fungus. Dermatophytes, yeasts, and molds are the most frequent forms of fungus to infect the toenail. Dermatophytes are the most common among the three. Symptoms associated with fungal nails include the discoloration of the toenail, brittleness, and in some circumstances, a smell. Pain is rarely a symptom caused by toenail fungus.
Diagnosis of fungal nails is generally a rather quick process. However podiatrists will make sure that the cause is not another condition such as lichen planus, psoriasis, onychogryphosis, or nail damage. Podiatrists will make use of fungal cultures and microscopy to verify that it is fungus.
While over-the-counter ointments are readily available, most are ineffective. This is due to the fact that the nail is very protective and that the fungus slips in between the nail plate and bed. Podiatrists can offer oral medication which currently provides the best results.
Ultimately, prevention is the best line of defense against toenail fungus. Avoid unsanitary public showers. If you do use a public shower, use shower shoes to provide your foot with protection. Once you are finished showering, make sure to thoroughly dry your feet. Fungi thrive in warm, dark, and moist places like sweaty, warm feet that are left dark in shoes all day.
Have I Broken My Toe?

Toe fractures are breaks or cracks in one or more of the small bones of the toes, often resulting from trauma, stubbing, dropping a heavy object on it, or sports injuries. Symptoms typically include pain, swelling, bruising, difficulty walking, and sometimes visible deformity of the toe. Risk factors that increase the likelihood of toe fractures include participating in high-impact activities, having weak bones, or wearing improper footwear that does not protect the toes. Untreated fractures can lead to chronic pain, joint stiffness, or improper healing. A podiatrist can accurately diagnose toe fractures, provide proper immobilization, recommend pain management, and create a treatment plan to ensure correct healing. If you think you have broken your toe, it is suggested that you promptly consult a podiatrist who can offer effective treatment solutions that are right for you.
Broken toes may cause a lot of pain and should be treated as soon as possible. If you have any concerns about your feet, contact Ambrose Su, DPM from Cascade Foot Clinic. Our doctor will treat your foot and ankle needs.
What Is a Broken Toe?
A broken toe occurs when one or more of the toe bones of the foot are broken after an injury. Injuries such as stubbing your toe or dropping a heavy object on it may cause a toe fracture.
Symptoms of a Broken Toe
- Swelling
- Pain (with/without wearing shoes)
- Stiffness
- Nail Injury
Although the injured toe should be monitored daily, it is especially important to have a podiatrist look at your toe if you have severe symptoms. Some of these symptoms include worsening or new pain that is not relieved with medication, sores, redness, or open wounds near the toe.
If you have any questions please feel free to contact our office located in Bend, OR . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.
What to Know About a Broken Toe
Trauma to the foot, especially the toes, can occur in many ways. Banging them, stubbing them, or dropping something on them are a few different ways this trauma can occur. Given the fact that toes are positioned in front of the feet, they typically sustain the brunt of such trauma. When trauma occurs to a toe, the result can be a painful break or fracture. Another type of trauma that can break a toe is repeated activity that places stress on the toe for prolonged periods of time.
Broken toes can be categorized as either minor or severe fractures. Symptoms of minor toe fractures include throbbing pain, swelling, bruising on the skin and toenail, and the inability to move the toe with ease. Severe toe fractures require medical attention and are indicated when the broken toe appears crooked or disfigured, when there is tingling or numbness in the toe, or when there is an open, bleeding wound present on the toe.
Generally, a minor toe break will heal without long-term complications. However, it is important to discontinue activities that put pressure on the toe. It is best to stay off of the injured toe and immediately get a splint or cast to prevent any more additional movement of the toe bones. You can also immobilize your toe by placing a small cotton ball between the injured toe and the toe beside it. Then, tape the two toes together with medical tape. Swelling can be alleviated by placing an ice pack on the broken toe directly as well as elevating your feet above your head.
Severe toe fractures may be treated with a splint, cast, and in some cases, minor surgery, especially when the big toe has been broken. Due to its position and the pressure the big toe endures with daily activity, future complications can occur if it is not properly treated. Pain associated with minor toe fractures can be managed with over-the-counter pain medications. Prescription pain killers may be necessary for severe toe fractures.
The healing time for a broken toe is approximately four to six weeks. In severe cases where the toe becomes infected or requires surgery, healing time can take up to eight weeks or more. While complications associated with a broken toe are immediately apparent, it is important to note that there are rare cases when additional complications, such as osteoarthritis, can develop over time. You should immediately speak with your podiatrist if you think you have broken your toe due to trauma. They will be able to diagnose the injury and recommend the appropriate treatment options.
How Corns and Calluses Differ
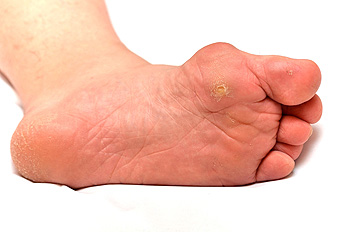
Corns and calluses both develop when the skin on the feet is exposed to repeated pressure, but they are not the same. A corn is a small, cone-shaped bump that often appears on the top of a toe, usually over a joint, and it can feel sore when touched. Corns between the toes are softer because the skin stays moist in that area. A callus is a wider, flatter patch of thick skin that often forms on the ball of the foot or the sides of the feet where weight and rubbing increase. Calluses rarely hurt unless they become very thick. A podiatrist can tell the difference by looking at the size, shape, and location of the hardened skin. Treatment options for a painful corn include reducing pressure on the toe, removing the hardened center, and safely trimming the thickened skin. If you have a painful corn on your foot, it is suggested that you schedule an appointment with a podiatrist for a diagnosis and safe, sterile treatment.
If you have any concerns regarding your feet and ankles, contact Ambrose Su, DPM of Cascade Foot Clinic. Our doctor will treat your foot and ankle needs.
Corns: What Are They? and How Do You Get Rid of Them?
Corns can be described as areas of the skin that have thickened to the point of becoming painful or irritating. They are often layers and layers of the skin that have become dry and rough, and are normally smaller than calluses.
Ways to Prevent Corns
There are many ways to get rid of painful corns such as wearing:
- Well-fitting socks
- Comfortable shoes that are not tight around your foot
- Shoes that offer support
Treating Corns
Treatment of corns involves removing the dead skin that has built up in the specific area of the foot. Consult with Our doctor to determine the best treatment option for your case of corns.
If you have any questions, please feel free to contact our office located in Bend, OR . We offer the newest diagnostic and treatment technologies for all your foot care needs.
Everything You Need to Know About Corns
Corns are hard and thick areas of skin that form as a result of constant rubbing, friction, or pressure on the skin. They are patches of dead skin with a small plug toward the center. They may appear on the tops and sides of toes and can make walking painful.
Soft corns are typically thinner with a white color and rubbery texture. Soft corns tend to appear between the toes. Seed corns are another type of corn that appear in clusters and can be tender if they are on a weight-bearing part of the foot. Seed corns usually appear on the bottom of the foot and are likely caused by a blockage in sweat ducts.
While corns and calluses are somewhat similar, calluses are a bit different. Calluses are a patch of dead skin that can occur anywhere on the body. In comparison to corns, calluses are usually a bit larger in size. However, both corns and calluses are caused by increased friction on the skin.
There are some risk factors that may increase your chances of developing corns and calluses. If you have bunions, hammertoe, or a bone spur, you are more likely to develop a corn or callus on your foot.
While Corns and Calluses tend to disappear when the friction to the affected area ceases, the help of a podiatrist may be useful in the removal process. It is important to remove the dead skin around the area and this may be done in a few different ways. Moisturizing creams may be helpful in softening and removing the dead skin around the callus. You should never use razors or other pedicure equipment to remove your corns. Doing this may worsen your corn or callus and cause infection.
In some cases, corns and calluses may be caused by abnormal foot structure or walking motion. In such a case, you should seek a podiatrist’s assistance in order to correct the issue.
Foot Neuropathy and the Risk of Falling
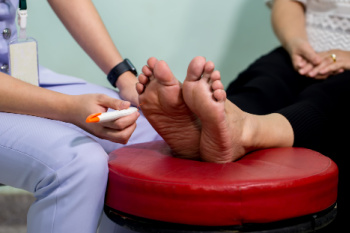
Peripheral neuropathy affects the nerves that carry signals between the feet and the brain. When these nerves are damaged, sensation in the feet may become reduced, altered, or unpredictable. People may not fully feel the ground, notice changes in surface texture, or sense foot position during walking. This loss of feedback can interfere with balance and coordination, increasing the risk of tripping or falling. Muscle weakness and slower reaction times can further add to instability. A podiatrist plays an important role in evaluating nerve function and identifying contributing factors. Treatment may include footwear guidance, custom orthotics, balance-focused exercises, and strategies to protect numb areas of the feet. Early care helps improve safety, maintain confidence with walking, and reduce fall-related injuries that can significantly impact mobility and independence. If you are experiencing neuropathy in your lower extremities, it is suggested that you visit a podiatrist for relief options.
Neuropathy
Neuropathy can be a potentially serious condition, especially if it is left undiagnosed. If you have any concerns that you may be experiencing nerve loss in your feet, consult with Ambrose Su, DPM from Cascade Foot Clinic. Our doctor will assess your condition and provide you with quality foot and ankle treatment for neuropathy.
What Is Neuropathy?
Neuropathy is a condition that leads to damage to the nerves in the body. Peripheral neuropathy, or neuropathy that affects your peripheral nervous system, usually occurs in the feet. Neuropathy can be triggered by a number of different causes. Such causes include diabetes, infections, cancers, disorders, and toxic substances.
Symptoms of Neuropathy Include:
- Numbness
- Sensation loss
- Prickling and tingling sensations
- Throbbing, freezing, burning pains
- Muscle weakness
Those with diabetes are at serious risk due to being unable to feel an ulcer on their feet. Diabetics usually also suffer from poor blood circulation. This can lead to the wound not healing, infections occurring, and the limb may have to be amputated.
Treatment
To treat neuropathy in the foot, podiatrists will first diagnose the cause of the neuropathy. Figuring out the underlying cause of the neuropathy will allow the podiatrist to prescribe the best treatment, whether it be caused by diabetes, toxic substance exposure, infection, etc. If the nerve has not died, then it’s possible that sensation may be able to return to the foot.
Pain medication may be issued for pain. Electrical nerve stimulation can be used to stimulate nerves. If the neuropathy is caused from pressure on the nerves, then surgery may be necessary.
If you have any questions, please feel free to contact our office located in Bend, OR . We offer the newest diagnostic and treatment technologies for all your foot care needs.